Bariatric Surgery
Robotic or Laparoscopic
2 weeks
1-2 hours
For individuals with a BMI > 37.5, this procedure is a way to reduce your exposure to illnesses like diabetes, high blood pressure, sleep apnea, gall stones and more.
Obesity is a condition of excess body weight i.e., when a person is 20% or more above the ideal body weight. Obesity results from a chronic positive energy balance regulated by a complex interaction between endocrine tissues and the central nervous system.
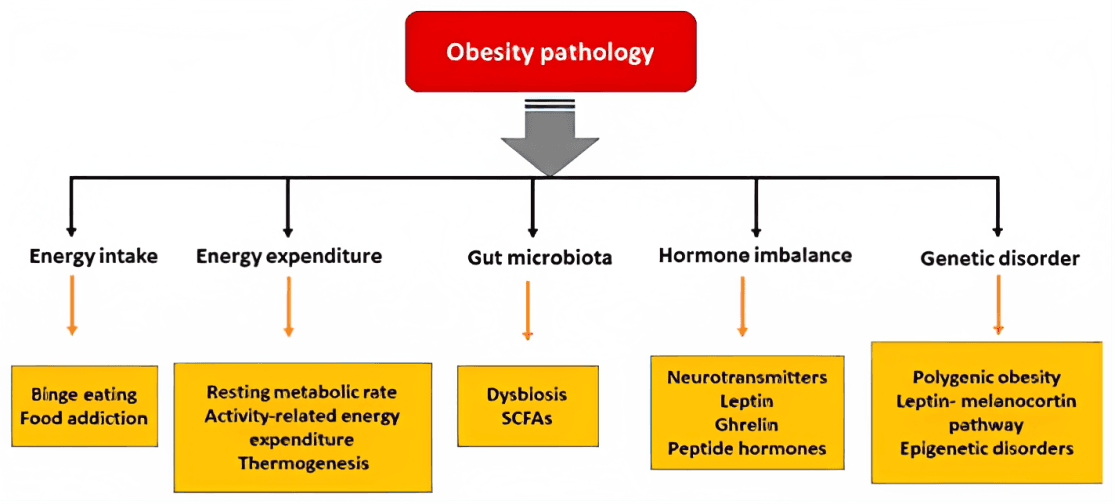
Do you think Obesity treatment is as simple as this?
Studies show that having a reduction in calorie intake as the central plank of an antiobesity strategy fails to acknowledge the existence of physiological mechanisms that predispose to its failure. Lower energy intake leads to hormonal changes that stimulate appetite (Lean & Malkova, 2016), reduces metabolic rate (Dulloo & Jacquet, 1998), and stimulates the consumption of more calorific foods (Benton, 2005)
Weight loss activates powerful compensatory biological pathways
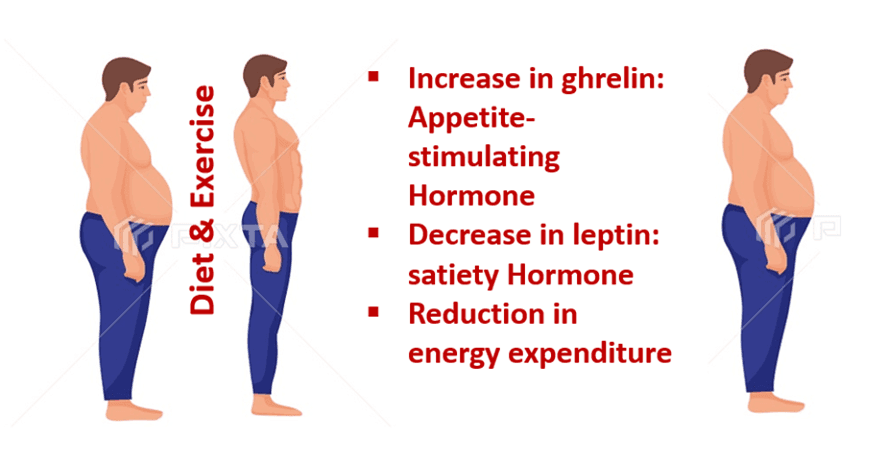
Bariatric surgery is a last resort for those who have not responded to diet, physical activity, and other non-surgical means of weight loss.
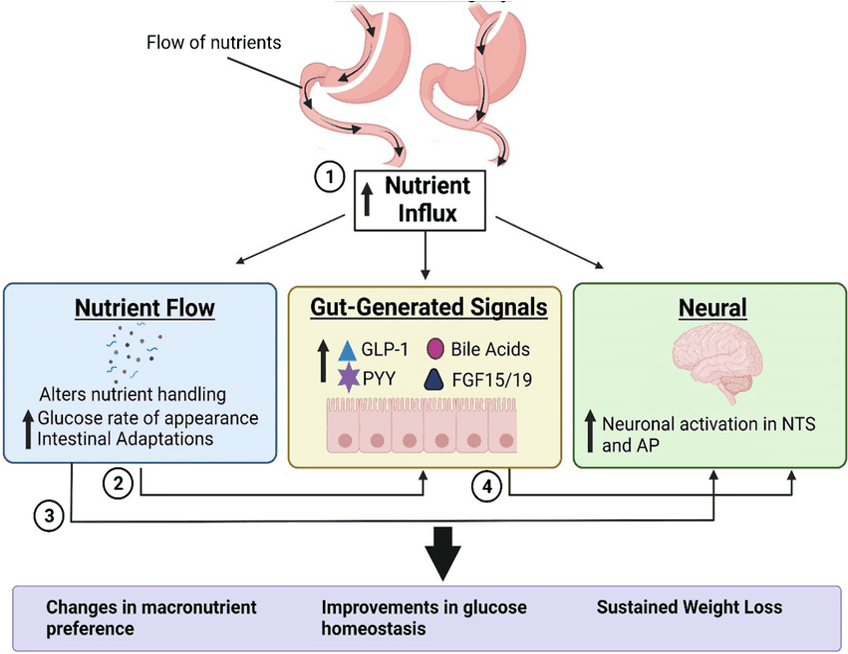
Bariatric surgery alters the gut brain axis and allows to lose substantial amount of weight and at the same time is switching off the hunger
Bariatric surgery together with a comprehensive assessment support and follow up program allows patients to achieve their target weight.
When we perceive people with who are suffering with obesity, we assume that these are people who have probably inflicted this upon themselves and they are responsible for their weight. We all need to realize that obesity is a disease like any other chronic progressive disease similar to diabetes or heart disease and the progression is similar as various stages.
Bariatric surgery is the most successful long-term treatment for obesity. it is nearly impossible for people with morbid obesity to sustain weight loss through diet and exercise alone. According to “Set Point Theory” once your body has registered your higher weight as “normal,” it continues to try to return to that weight.
Bariatric surgery works by changing how your body manages what you eat, allowing healthy diet and lifestyle changes to be effective for sustained weight loss and health. Bariatric surgery remains the only effective and enduring treatment for morbid obesity.
Bariatric surgery is basically a gastrointestinal surgery where there is an alternation a in the GI tract and this surgery is a last resort for those who have not responded to nutrition, physical activity, and other non-surgical means of weight loss.
Many of the hormonal signals that cause weight gain or inability to lose weight are affected by these procedures, and it becomes easier to lose weight. But this still requires a healthy diet and a good exercise routine. These procedures are tools to treat a chronic disease, and cannot work alone.
Bariatric surgery is the last line of treatment for obesity and related diseases along with increased life expectancy and enhanced quality of life.
Patients suffering from morbid obesity should undergo Bariatric Surgery to -
Reduce life threatening risk factors
Improve self-esteem
Enhance quality of life
Mechanism of Bariatric Surgery
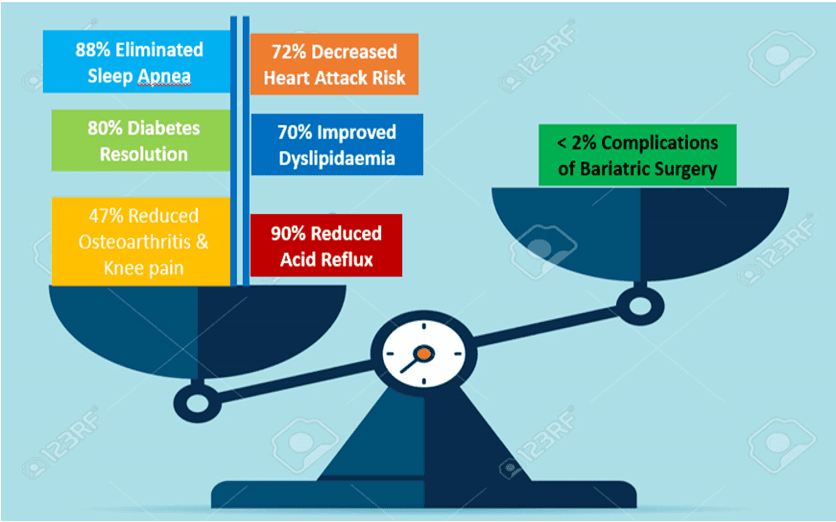
Risk of positive benefits of bariatric surgery vs complications
Eligibility Criteria for Bariatric Surgery
Today we actually can define the stages of the obesity on the basis of body mass index a parameter to define the stages of obesity
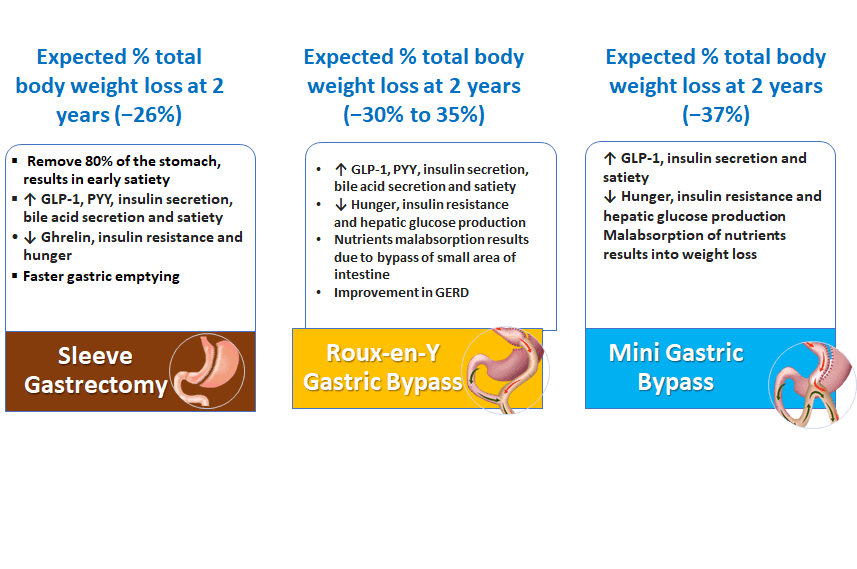
Sleeve Gastrectomy:
Roux-en Gastric Bypass
Roux -en-Y Gastric Bypass is a combination of restrictive and malabsorptive technique which enhances the surgery outcomes
This procedure restrict the calories intake (Restrictive Procedure) and at the same time limit the food absorption (Malabsorptive procedure)
STEP 1
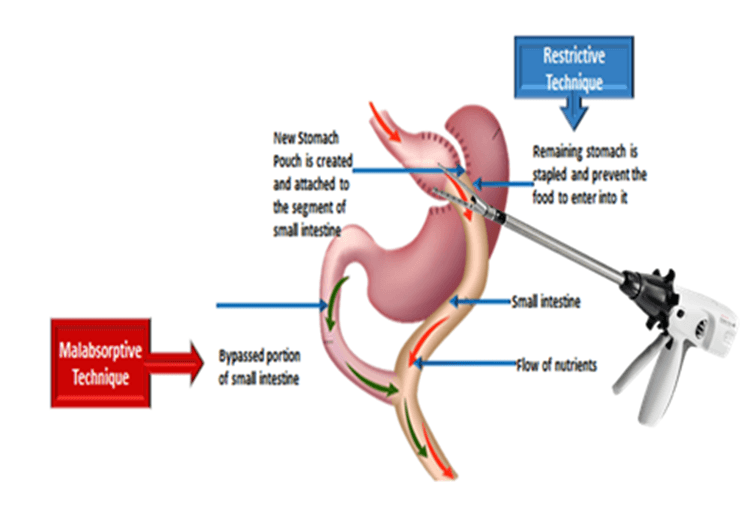
Roux-en-Y Gastric bypass surgery is a procedure where small portion of the upper portion of the stomach near oesophagus is separated from the rest of the stomach and a small pouch is created by stapling (This causes food restriction)
STEP 2
The lower segment of the intestine joined to the small pouch of the stomach (Malabsorption). The upper segment of the intestine which carries digestive juices from the remnant stomach re-attached at the distal end of the rouex limb by stapler or by suturing, thereby diversion of bile as well as intestinal secretion. In this procedure depending on the BMI approx. 125 -170cm of the small intestine is bypassed
Mini Gastric Bypass
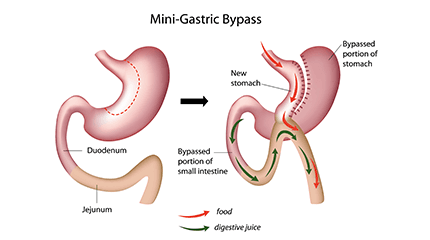
Mini gastric bypass is simpler procedure as compared to Roux en gastric bypass as it involves less rerouting of intestine, single anastomosis and comparatively less surgery time.
Mini Gastric Bypass procedure combines the effect of restriction and malabsorption to lose weight. The upper portion of the stomach is created into a long gastric tube and a wide loop of the small intestine is sutured with the gastric tube , bypassing approx. 150-200 cm of intestine , which causes malabsorption effect.
The restrictive technique reduces the gastric capacity and induces early satiety, which causes less consumption of food
By contrast, the malabsorptive technique involves malabsorption of the food and alteration of the gut hormones which can improve metabolic diseases like fatty liver. Insulin resistance, glycemic control
Single anastomosis sleeve ileal bypass (SASI)
SASI bypass is a novel bariatric procedure that reaches a compromise between the effect of restriction and malnutrition. This procedure utilizes neuroendocrine mechanisms that bind the alimentary tract and the nervous system. Single anastomosis sleeve ileal bypass (SASI) surgery is divided into 2 parts:
The first stage is gastric sleeve resection, which supports weight loss by mechanism of restrictive procedure
The second stage is the sleeve ileal bypass, where undigested aliment reaches the ileum fast and trigger the good hormone release from the distal ileum. Modification of the intestinal transit changes the concentration of orexigenic and anorexigenic hormones. When the undigested food is introduced to the lower portion of the small bowel, a hormone is produced to send the information to the brain to stop the appetite by slowing down the peristalsis and gastric emptying.
Food can pass through the duodenum and the jejunum, so this mechanism can reduce the negative effects of malabsorption. SASI-S also minimizes the risk of long-term nutritional problems and reduces reflux by dropping the pressure in stomach.
It benefits from the effect of fast transit of indigested food to the ileum, where anorexigenic intestinal hormones are released.
Apart from weight loss, the effect of SASI bypass is a rapid resolution of diabetes
The advantage of SASI bypass is more term of diabetes resolution
Advantages of SASI-S Surgery:
Early satiety and less hunger due to reduction in ghrelin production
Food can pass through the duodenum and the jejunum, so there is less malabsorption and lower risk of nutrition deficiencies in long term
Access to bile duct is easily available
Modification in the intestinal transit can give extra advantages in 70-90% diabetes resolution
Less risks of internal hernia
Less incidence of weight regains
Positive impact on acid reflux as pressure on the stomach is reduced
Indications of SASI-S Surgery
Patients with BMI greater than 40
Patients with BMI 35 and have one or more co-morbidities such as: Type 2 diabetes, sleep apnea, insulin resistance, dyslipidaemia and cardio vascular diseases
SADI- S or SIPS Surgery
SADI -S or SIPS Surgery also known as One anastomosis duodeno-ileal switch or stomach intestinal sparing surgery
SADI -S is a combination of sleeve gastrectomy and duodenal switch surgery. This procedure involves two steps:
In the first step surgeon creates a sleeve like gastric sleeve gastrectomy, where 80% of the stomach is removed which reduces the food intake.
The second step of a SADI-S procedure involves creating the bypass where the surgeon will detach the intestine below the stomach and reattach it about 2 metres down. This way, food will bypass the part of the digestive tract that absorbs most nutrients and calories, and produces malabsorptive effect for weight loss, good glycemic control which helps in diabetes resolution,
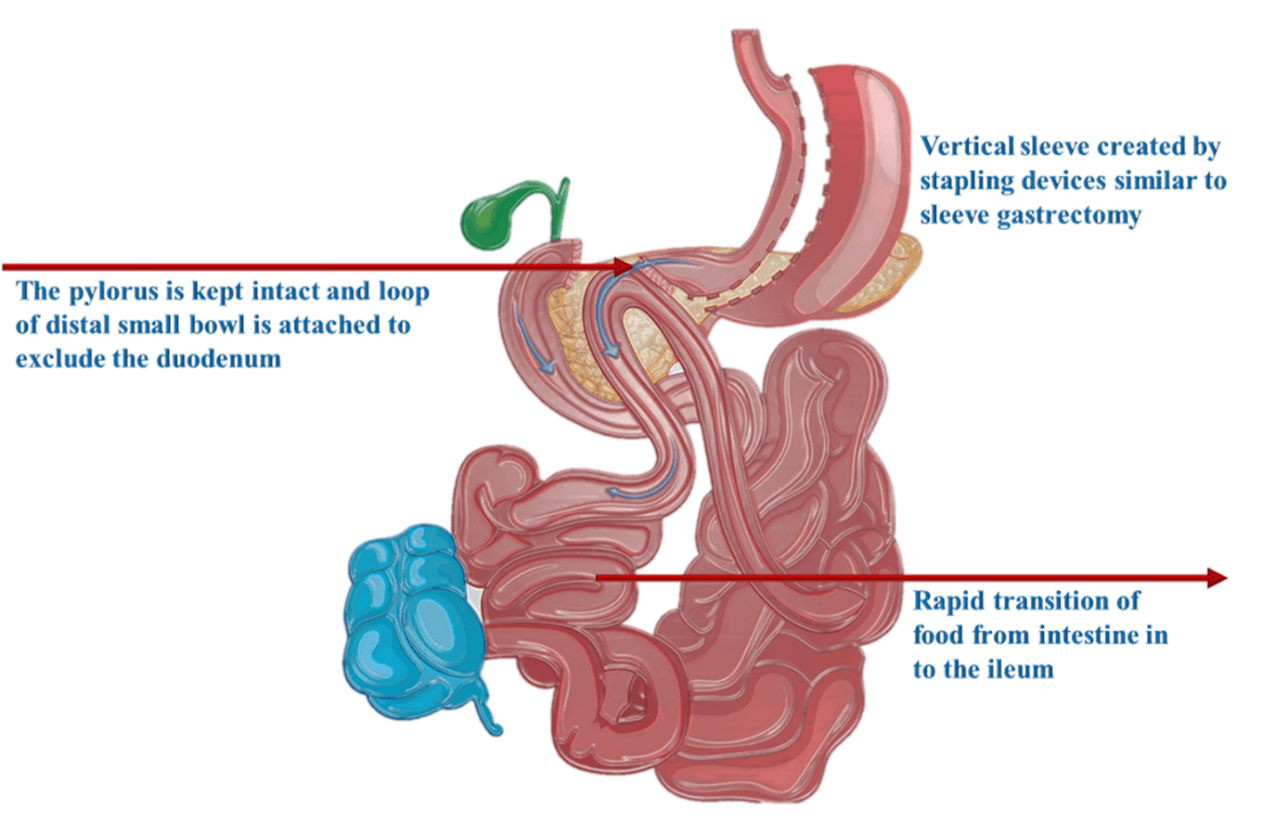
Advantage of SADI-S surgery:
• This procedure results into significant weight loss and results in 80-90% of excess weight loss
• Diabetes resolution.
• Low incidence of dumping syndrome
• Minimal risk of ulceration at anastomosis site.
Endoscopic Sleeve Gastroplasty (ESG)
Endoscopic sleeve gastroplasty is an innovative technique used as a bridge between conventional weight loss method and bariatric surgery. This procedure is a non-invasive procedure for obesity treatment. In this procedure the volume of the stomach is reduced by endoscopic suturing, which guarantees a reduced complications rate.
Mechanisms of weight loss post Endoscopic sleeve gastroplasty:
Endoscopic sleeve gastroplasty procedure generates preventive satiety due to sewing of part of stomach that produces hunger hormone.
Endoscopic sleeve gastroplasty slows down the gastric emptying of the stomach and reduces hunger.
Indications of bariatric surgery:
In morbid obese patients where, bariatric surgery is contraindicated can be performed as a primary procedure.
Endoscopic surgery can be performed as a revisional surgery in patients with inadequate weight loss or patient who needs revisional bariatric surgery
Patient with chronic diseases like liver diseases, renal diseases with obesity can undergo this procedure to reduce weight and to delay the progression of the disease
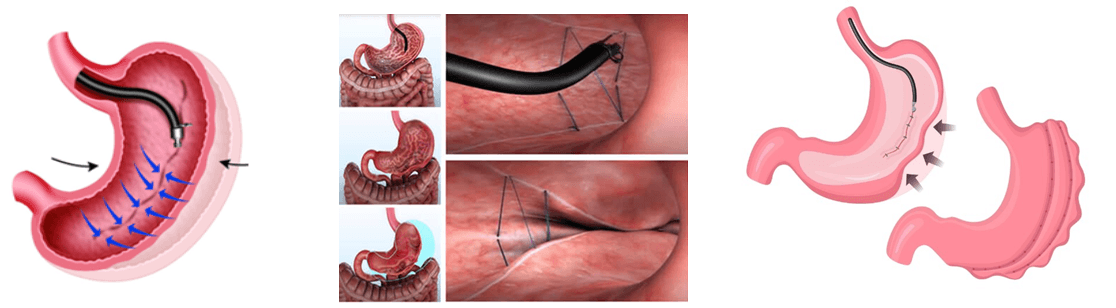
Essential steps for performing ESG
A comprehensive pre procedure investigation and preoperative counselling session by surgeon, dietitian, and psychologist
Procedure performed under general anaesthesia with endoscope and special suturing device i.e. Apollo Overstich device, which is a long and flexible tube with a camera and a set of suturing tools
Surgeon insert the Overstich device through the patient’s throat into the stomach and sews a series of internal sutures in the stomach wall. This reduces the size of the gastric cavity and prevents its distension
Procedures takes 60-90 minutes
One day hospitalisation for pain management, hydration and maintaining vitals
A special diet for 1 month prescribed by qualified dietitian
A vigorous follow up is essential
Advantages of endoscopic sleeve gastroplasty
Endoscopic sleeve gastroplasty ensures faster recovery and less pain
Patient can resume their work within 3 days after procedure
Patient can loose 25 to 30% of excess body weight
Procedure is reversible
The protocol before the operation is:
Preoperative Exams: Blood investigations, X ray, ECG
Bariatric Surgeon Counselling:
In order to exclude contraindications, to understand the pros and cons of the procedure
To know the post procedure management, expectations, and post operative follow up protocol
Surgeon should know the medical history and associated disease condition, so that procedure should not be affected by these conditions.
Psychiatrist Counselling:
It is essential to exclude any psychiatric illness, eating disorder or substance abuse
2, To evaluate the willingness of the patient for lifestyle modifications to enhance the efficacy of the procedure
Dietitian Counselling:
To learn the healthy way of eating, portion size , requirements of energy and protein
As this is a restrictive procedure so patient counselling is essential to avoid deficiency of any micro nutrients
Similar to any bariatric procedure, the patient should learn to do mindful eating, regular follow up for nutrition monitoring, regular physical activities and behaviour modification.
Intragastric balloon
Intragastric balloon is non invasive procedure of treating grade 1 and grade II obesity or a bridging procedure in super obese patient to lose weight for preparing the patient for bariatric procedure
This procedure is also suitable for those patients who are not falling under bariatric surgery criteria but suffering from obesity related diseases.
This procedure involves introducing a silicon balloon in the stomach through endoscope and filling it with liquids with the capacity of 500-600 ml which remain in the stomach for 6 months. In most of the patients it is a day care procedure but in few cases one day hospitalization is required
This procedure is a restrictive procedure, as a result patient consume less food which results in weight loss.
Intragastric balloon procedure is associated with low risk. Patient can resume daily activities within 5-7 days.
Patient can loose 12-15 % of excess body weight that depends upon factors like weight, excess body fat, diet and physical activities
This procedure is effective in those patients who are highly motivated and after balloon removal willing to maintain the life style modifications
Patient should follow rigorous diet and exercise program in order to achieve the best result.
The gastric balloon placement:
The gastric balloon is inserted inside the stomach through an endoscope. Once the balloon reaches inside the stomach it is filled with a sterile solution, which allow the balloon to float freely inside the stomach
The procedure is performed under anaesthesia to avoid any discomfort or pain and it take 20-30minutes to perform this procedure
After discharge patient can resume their normal activities.
In general, patient can feel some gastric discomfort, nausea and omitting after the treatment. Follow the discharge medications and suggested diet.
After 6 months balloon can be removed endoscopically under sedation and this procedure can take 15-20 minutes
The advantage of this procedure is that it regulates the eating behaviour and prevents overeating without any surgical intervention
Gastric Balloon procedure improves the quality of life by addressing the obesity related diseases like
Gastroesophageal reflux disease.
High blood pressure.
Coronary artery disease.
High cholesterol.
Obstructive sleep apnea.
Type 2 diabetes.
Osteoarthritis and general joint pain.
Nonalcoholic fatty liver disease.
Contraindications of Gastric Balloon:
Previous gastrointestinal surgery
The presence of a large hiatal hernia, or a bleeding lesion of the upper digestive tract.
Bleeding disorder, active alcoholism or drug addiction, and important liver disease.
Pregnancy
Some medications
Psychiatric diseases.